In December 1994 then former U.S. surgeon general C. Everett Koop launched a national weight-loss campaign at a White House press conference, stating that obesity had become the country’s second-largest cause of death, “resulting in about 300,000 lives lost each year.”
This marked the beginning of a long, influential life for the statistic. Pundits and scientists alike began citing the number to highlight the gravity of the “obesity epidemic.” It was leveraged in Food and Drug Administration approval hearings for weight-loss medications with questionable safety profiles. One drug, dexfenfluramine (Redux), was later pulled from the market for damaging patients’ heart valves. Another, sibutramine (Meridia), was removed for increasing the risk of heart attacks and strokes.
After a decade the number had ballooned to nearly 400,000 deaths attributed to high weight, with predictions that it would soon reach half a million—about 20 percent of all annual American deaths. But by 2005 these seemingly staggering numbers were overturned. The statistic slayer was Katherine Flegal, then a senior scientist at the Centers for Disease Control and Prevention and now one of the most cited epidemiologists in her field.
Hoping to better understand the relationship between body size and mortality, Flegal led a study that ultimately revealed something many scientists—and certainly the public—did not expect: the annual deaths related to obesity tallied to just more than 100,000. More interesting still, people considered clinically “overweight” had a longer life expectancy than those who fell in the “normal” weight category. (So if you added the overweight and obese categories together like in previous studies, the total was under 26,000 deaths).
Her work should not have caused such a stir. It was consistent with other research and backed by the CDC (it even received a 2006 Charles C. Shepard Science Award, one of the agency’s most prestigious honors). Yet the study was met with a firestorm of doubt and criticism.
“People were preemptively contacting journalists saying that our article was rubbish,” Flegal says. “Our findings produced controversy because someone wanted a controversy.”
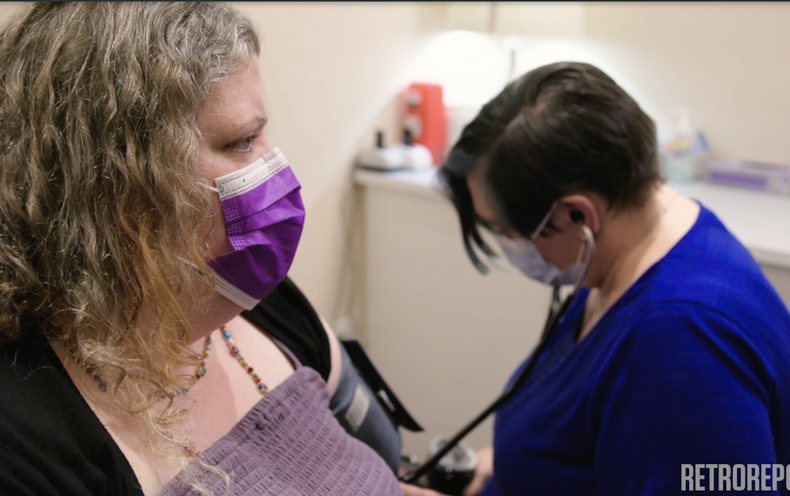
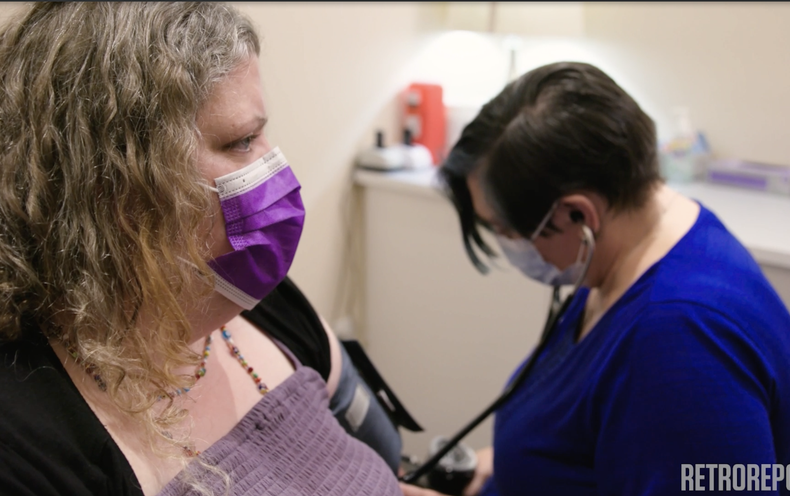
In this short documentary, Retro Report partners with Scientific American to examine how biases about body size can influence the questions scientists investigate and what information people accept as true.
Myths, assumptions and biases are persistent and well documented in the contentious realm of obesity research. Flegal says they are bolstered by societal weight stigma and the financial interests of the pharmaceutical and weight-loss industries. “The whole area of body weight and obesity has become very, very difficult to study objectively,” she explains. “There’s so much emotion, so many interests that are involved.”
As an example of the stubbornness of ingrained beliefs about obesity, the infamous “300,000 deaths” statistic still lives on today despite the lack of supporting evidence. In the past year alone it has appeared in opinion pieces from the Hill, the Washington Post and a variety of local newspapers. (Most have cited a Web page by the West Virginia health department’s Health Statistics Center that has not been updated since 2003).It has also been referenced recently in top medical journals, health manuals and even a congressional bill. Plus, it is a favorite of weight–loss centers across the country.
“People are just more comfortable with a larger number—they prefer it to be larger,” Flegal suspects. “I don’t think discomfort itself should be a factor in science, but I think it has more of an effect than we might realize.”
Bias muddies the process of science. And in nutrition science and medicine, that bias can often equate to the idea that thinner is better, skinnier is healthier. And when results seem to contradict that preconceived notion, the findings are often qualified by the phrase “obesity paradox.”
“You can report the same findings about obesity 100 times, and it can be called ‘unexpected’ every single time,” Flegal says. “It’s like, well, at what point would you change your mind and say this might be the expected result?”
So far this so-called paradox has been documented in several conditions, including heart disease, lung cancer, type 2 diabetes and stroke, among others. But the label of “obesity paradox” can often lead to disbelief around such results even though they present an opportunity to learn something new, says Bette Caan, a cancer researcher at Kaiser Permanente, who stumbled onto her own “paradox” in breast cancer.
“It’s human nature for people to find evidence that supports their belief,” Caan says. “We need to study where the data takes us.” Her own “unexpected findings” led to a discovery that could impact breast cancer patients across the nation: retaining muscle during treatment is far more important to survival than avoiding weight gain.
“We can’t be stuck in what we thought was true,” Caan says, “because then we’re never going to move the field forward.”